Hot Topic!
Winter 2024
The holidays are over, you may have gained some weight and feel like you have less energy. You may also feel like you have the “winter blues” but this might be more than just a feeling.
You may be experiencing Seasonal Affective Disorder or SAD.
Seasonal affective disorder (SAD) is a type of depression that’s related to changes in the season usually starting in the fall and winter months. Unfortunately, the colder weather and less sunlight can affect our emotions.
Some signs and symptoms of SAD may include:
- Feeling listless, sad or down most of the day, nearly every day
- Little or no interest in activities you once enjoyed in the cold weather
- Low energy and feeling like you are slow-moving
- Problems with sleeping too much
- Diet changes like carbohydrate cravings, overeating and weight gain – especially after the holidays
- Difficulty concentrating
- Feelings of hopeless, worthless or guilty
Causes of seasonal affective disorder are unknown some factors include:
- Your internal biological clock called circadian rhythm can be off. The decrease in sunlight can interrupt your body’s internal clock and lead to increased depressed feelings.
- The decreased sunlight can cause a reduction in serotonin, one of the brain’s neurotransmitters, which can trigger depression.
- The change in season can ultimately disrupt the balance of the body’s level of melatonin, which helps our sleep patterns and mood.
Some treatment options for SAD can be light therapy, psychotherapy and sometimes medications. Other treatments include doing things that you enjoy, going outside in the sunlight, spending time with family and friends and eating healthy foods, avoiding increased sugary foods and carbohydrates.
There’s no known way to prevent the development of seasonal affective disorder. However, if you take steps early to help manage symptoms, you may be able to prevent them from getting worse over time.
If you feel like you have the “winter blues” or a seasonal funk that you don’t always have – you don’t have to feel like you need to tough this out on your own. Speak to a provider at your next visit.
Happy New Year!!!
Maryanne
February 2023
What Virus Is It?
I think I have the Flu or is it Covid.
You may have RSV (Respiratory Syncytial Virus)!
RSV is the leading cause of lower respiratory tract infections in infants and very young children. Approximately4-5 million cases are diagnosed in the U.S.A. every year. It also causes about 175,00 hospitalizations in the elderly >65 years annually.
As temperatures decline in the fall, RSV season starts to ramp up. This year we saw an unusually high number of cases early in the fall. Health officials feel the early surge is due to multiple factors. Lifting the Covid restrictions has caused greater exposure again to all viruses. Also, infants born during the pandemic have not been regularly exposed to the RSV virus and may now be more susceptible to infection. Surprisingly we have also seen an increase in the number of symptomatic adults to help fuel the surge.
Most cases of RSV in adults present as mild cold symptoms of cough, congestion and low fever. In infants more severe cases present with wheezing, shortness of breath, heart racing and cyanosis. Severe cases can lead to pneumonia and sepsis in infants and the very old.
Treatment for the most part is symptomatic control. In mild cases that includes staying well hydrated and keeping nutrition up. Fever control with antipyretics and cough/decongestant meds. Cases leading to hospitalizations my require bronchodilators, alpha agonists and oxygen.
Precautions such as hand washing, avoiding touching our face and disinfectant sprays can be of benefit. The best defense is keeping our newborns and infants away from those who are sick or recently sick. Unfortunately, many adults can be carriers of the virus and spread to those more susceptible.
There is no vaccine for the RSV virus at present. There are injectable immunoglobulins like Palivizumab to give high risk infants monthly during RSV season to help protect infants.
The goal is to protect our most vulnerable in the population, our very young and old. Lets wash our hands , use hand sanitizer when not able to, stay away when we’re not feeling well. There are more things out here than Covid and the Flu that can cause harm, help prevent the spread of RSV.
January 2023
Have you ever had sleepless nights?
Have you ever gone to bed but then wake up and can’t fall back to sleep?
Yes you say, then you are not alone, this is called insomnia and it’s a common term for those who can’t fall asleep or have trouble falling asleep and staying asleep.
Insomnia can be acute or chronic, many adults and now children, experience short term or acute insomnia.
Acute insomnia can be related to stress or a traumatic episode. Others can experience long term or chronic insomnia which can last for a month and even longer sometimes.
Insomnia can occur in males, females, adults and children.
The American Academy of Sleep Medicine and the Sleep Research Society recommend adults sleep at least 7 hours a night but over 25% of all adults do not meet this recommendation and this number has been rising since the start of COVID 19.
Some common causes of insomnia:
- Stress – Worries about work, school, health, which has been a huge factor since the start of COVID 19, also finances or family can keep your mind active at night. Stressful life events or trauma, such as a death or illness of a loved one again on the rise since COVID 19, divorce, and relationships.
- Work schedule -Your circadian rhythm which is an internal clock, controls your sleep-wake cycle, metabolism and body temperature can be changed with shift work or changing shifts. Disrupting that rhythm can lead to sleep issues.
- Poor sleep habits -Having irregular bedtime schedules, naps, stimulating activities before bed, an uncomfortable sleep environment, and using your bed for work, working on Computers, TVs, video games, smartphones or other devices just before bed can change your sleep cycle.
- Eating -Having a light snack before bedtime is OK, but eating too much may cause you to feel physically uncomfortable while lying down.
- Health conditions– some conditions linked with insomnia are chronic pain, cancer, diabetes, asthma GERD or reflux, heart disease, overactive thyroid, Alzheimer’s and Parkinson’s. Mental health conditions like anxiety disorders, PTSD, depression can often occur with sleep complaints.
- Medications -Some medicines can affect sleep, some antidepressants, and some medications for asthma or blood pressure. Also some over-the-counter medications like pain medications, allergy and cold medications, also some weight-loss products can contain caffeine and other stimulants which can cause a disruption in sleep.
- Sleep–related disorders – Sleep apnea can disrupt sleep due to the stopping of breathing periodically. RLS or restless leg syndrome causes sensations in your legs and also disrupt sleep.
- Caffeine, nicotine and alcohol -Coffee, tea, cola, and chocolate are all stimulants. Consuming them later in a day can hinder you from falling asleep at night. Nicotine or tobacco products are another form stimulant that can interfere with sleep. Alcohol may help you fall asleep, but it prevents deeper stages of sleep and this often causes disruption throughout the night.
Insomnia can become worse as we age with changes in our sleep patterns, napping more, reduced activity and unfortunately some may have more chronic health issues with increased daily medications.
Some risk factors associated with insomnia are:
- Being over age 60.
- Having mental health conditions or physical health disorders.
- Stressful times and events can cause temporary insomnia, any major or long lasting stress can lead to chronic insomnia.
- Irregular schedule either work or home, changing shifts at work or traveling can disrupt your sleep-wake cycle.
- Women have hormonal shifts during the menstrual cycle and in menopause which can play a role. During menopause, hormone swings can cause night sweats and hot flashes often disrupt sleep. Insomnia is also common with pregnancy.
Sleep is as important to your overall health as is a healthy diet and regular physical activity. Whatever your reason for sleep loss, insomnia can affect you both mentally and physically.
What are some treatments?
- CBT or cognitive behavioral therapy, training your brain to change the thought pattern of sleep and any negative thoughts surrounding sleep.
- Stimulus control therapy, set a consistent bedtime.
- Relaxation therapy, listen to music, controlled breathing.
- Sleep restrictions, avoid daytime naps.
- Medications, Eszopiclone (Lunesta), Ramelteon (Rozerem), Zaleplon (Sonata), Zolpidem (Ambien, Edluar, Intermezzo, Zolpimist). Over the counter medications such as Melatonin can also help.
So what can you do to help prevent or minimize insomnia?
- Keep your bedtime consistent even on weekends or days off
- Keep moving regular activity helps with a good night’s sleep.
- Check your medications to see if they may contribute to insomnia.
- Avoid or limit caffeine, alcohol, stop nicotine and avoid naps when you can
- Only small snack and beverages before bedtime.
- Make your bedroom comfortable for sleep not work
- Create a calming bedtime ritual, destress, read, listening to soft music
- Do whatever relaxes you!
If you feel you are struggling with acute or chronic anxiety mention it to your provider at your next visit!
Sleep well!!
Maryanne
December 2022
Holiday Heart Syndrome
It would not be unusual for anyone to celebrate the holidays with an adult beverage or two, eat too much of the once-a-year holiday treats either sweet or salty, then have a few more adult beverages and participate in the excitement or even stress of the holiday party. All sounds like a typical December event…..until it’s not!
So, what can go wrong? There is a very under publicized heart risk called Holiday Heart Syndrome which refers to a heart problem that involves overindulging in salty foods, alcohol, and caffeine, along with the stress or excitement of the day that culminates into an irregular heartbeat called Atrial Fibrillation ( A-fib). Although this irregular and often rapid heartbeat can occur anytime a person overindulges, the most common time is the Holiday season. Atrial Fibrillation besides making one feel like their heart is jumping out of their chest, can lead to serious heart issues like congestive heart failure, blood clots, and stroke. A person does not have to have underlying heart disease to have this happen, which means it could happen to you or any family or friends without warning.
The term Holiday Heart Syndrome was coined in 1978 due to the sudden onset of emergency room visits due to irregular heart rhythms which were found to be A-fib. This expression has stuck ever since.
What are the typical symptoms?
- Heart palpitations- a sudden pounding or fluttering or racing feeling in your chest
- Sudden tiredness or fatigue
- Chest pressure or pain
- Trouble breathing
- Feeling anxious
- Lightheadedness
If these symptoms in the circumstances of partying during the holiday season occur and last more than one hour after hydrating with water and stopping drinking alcohol, you should seek emergency room attention!
Prevention
Since alcohol is the main trigger Holiday Heart Syndrome, limiting the number of drinks you have in a short period of time would be the most obvious. Since alcohol can be very dehydrating, and dehydration can add to the risk of A-fib, making sure you are hydrated before and during the party. One glass of water then one alcoholic drink, repeat. Limit the salt and chocolate you consume during the party. The first bite and the last bite taste the same – these are treats for the holiday, so you don’t have to have five. And finally avoid those big controversial family discussions until after the holiday. Stress is not a gift that should be shared at this time of the year.
Remember the HOLIDAYS ARE TO BE ENJOYED, JUST NOT IN THE EMERGENCY ROOM!
Happy Holidays,
Dr. Lee Ann
Fall 2021
Covid Long Haulers
What happens when Covid-19 don’t go away? In some people symptoms can linger and wreak havoc for months. This is often referred to as Long Covid or Long Haulers.
In such patients the virus is no longer detectable in their system, but symptoms can be debilitating. Certain risk factors may make severe Covid more likely but there is no link between risk factors and long- term problems. It can even happen in people with mild symptoms.
Lasting symptoms can include fatigue, shortness of breath, cough and joint aches. Often cognitive memory problems include difficulty concentrating, depression and brain fog.
Long-term damage can occur to the lungs, heart, kidneys and brain. Mental health issues like anxiety and depression are common long-term effects. The sheer volume of covid cases makes this a challenge for health care providers to be able to reach all those suffering long-term effects. Especially when patients are fearful of coming in to see providers.
When it comes to Covid -19 how long is long-term? The answer is unknown at this point. Most people are less than one year out from their infections/recovery. Time will only tell how long is long.
Treatment entails addressing the symptoms that people have. A multi-disciplinary approach to support patients. Physical therapy, medicines, breathing therapy and mental health support can help speed recovery, but it may be a slow process. Seeking treatment is important as many symptoms can be similar to other disease processes. It’s important to rule out other medical issues as well.
Feel free to contact our office if you think you have Long Hauler symptoms.
Healthfully Yours Pine Street Family Practice
Dr. Steve
Spring/Summer 2021
Meditation can be a great way help reduce stress and improve one’s focus!
Here is a link that can be a first start for beginners. https://www.mindful.org/how-to-meditate/ or follow the instructions below.
Meditation is simple and hard at the same time. It sounds easy but needs practice to fully feel the affect.
Read these steps, make sure you’re somewhere where you can relax into this process, which can be difficult in this very busy different time, set a timer for yourself, and give it a shot:
1) Take a seat and find a comfortable calm place to sit that is quiet.
2) Set a time limit if you’re just beginning, it can help to choose a short time, such as five or 10 minutes. I recommend 5 minutes to start.
3) Notice your body, you can sit in a chair with your feet on the floor, or sit loosely cross-legged on the floor, you can kneel, whatever makes you comfortable but make sure you are stable and in a position you can stay in for a the 5 minutes.
4) Feel your breath, follow the feeling of your breath as it goes in and as it goes out really pay attention, it can be fascinating and so relaxing.
5) Notice when your mind has wandered, this I find is the most difficult part, when you get around to noticing that your mind has wandered, stop wait a few seconds, and return your attention to breathing.
6) Be kind to your wandering mind, don’t beat yourself up or obsess over your thoughts you find yourself lost in, work, kids, bills, job, no time, Just come back and try again, remember it takes practice!
7) Close with kindness, this is important? When you’re ready, gently lift your gaze (if your eyes are closed, open them). Take a moment and notice any sounds in the environment. Notice how your body feels at that moment along with your thoughts and emotions.
That’s it! That’s the practice. I would recommend twice a week at first even though 5 minutes isn’t a long time you may become frustrated until you really perfect it! Don’t give up!!
Remember take time for yourself in this busy time, if you have any questions, ask a provider at your next visit at Pine Street Family Practice!
Winter 2021
What is this COVID-19 Vaccine??
Moderna and Pfizer-BioNTech have produced a vaccine to help protect against the COVID-19 virus.
Pfizer-BioNTech’s vaccine is recommended for age 16 and older, administered into the muscle, a two-series vaccine administered 21 days apart from each other.
Moderna’s vaccine is recommended for age 18 and older, also administered into the muscle, also a two vaccine series administered 28 days apart from each other.
After administration you will be asked to sit and wait 15 minutes while medical personnel monitor you for any side effects.
Both vaccines are lipid particle mRNA vaccines encoding the prefusion spike glycoprotein of SARS-CoV-2, the virus that causes COVID-19. This is somewhat technical so here is how it works….
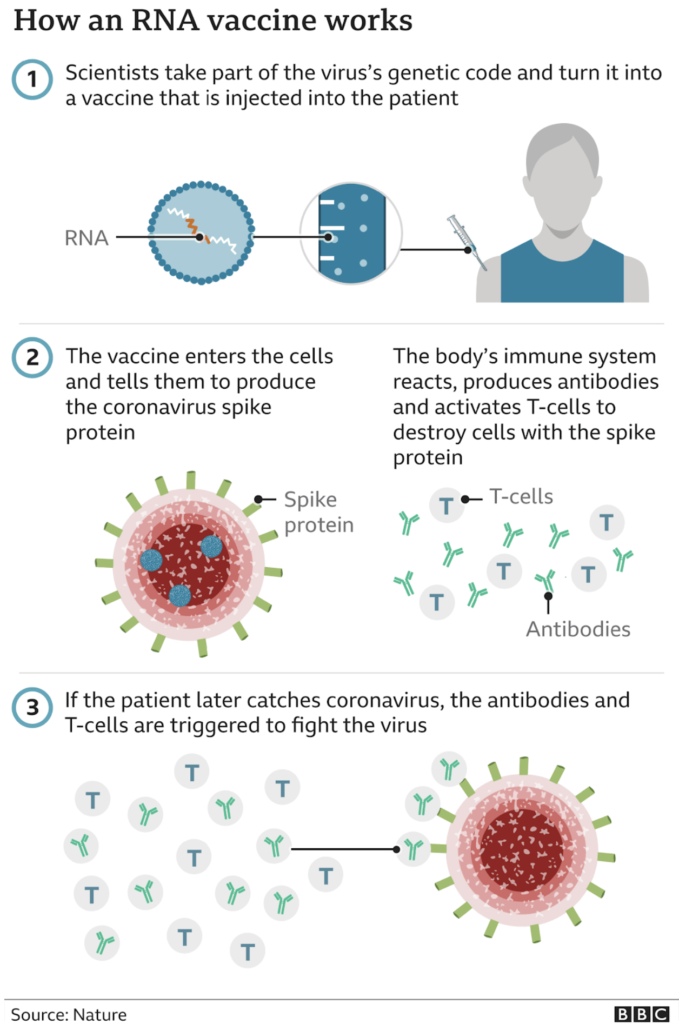
The need for and timing of future booster doses for the COVID-19 vaccine has not been established. No additional doses beyond the two dose primary series that are being distributed now are recommended at this time.
Antibody testing is not recommended at this time to check immunity to COVID-19 following vaccination.
It is recommended that vaccination should be deferred for at least 90 days if diagnosed positive with COVID-19.
Data suggests high vaccine effectiveness in preventing COVID-19, following receipt of the two doses Pfizer-BioNTech’s vaccine at 95.0% and Moderna’s at 94.1%. Limited data are currently available regarding the efficacy of a single dose. Which is why it is very important to complete the two-dose series to boost protection.
There is a link on our website that you can click on which will help direct you on how to register for your Covid vaccine.
Stay safe, wash your hands, wear your mask, keep 6 feet from others and get your two-series COVID-19 vaccine!
Fall 2020
The Most Effective Workouts for the Casual Exerciser
Attention all couch potatoes, lethargic loungers, and leisure lovers: You probably need a little more physical activity in your routine. But, that doesn’t necessarily mean you need to buy a gym membership, join a running club, or take up some extreme sport. If you like to take things slow or prefer the comfort of your own home (particularly during pandemic times), there are a number of exercises that might be closer to your speed.

These exercises have been scientifically proven to produce serious benefits without a serious commitment.
You may even be surprised to learn that some of these more gentle forms of exercise can provide a great boost to your physical health. According to a study published in The Journal of Physiology this year, even passive stretching can provide health benefits. The study examined how 12 weeks of passive leg stretching affected vascular function and arterial stiffness. The authors found that this simple stretching regimen led to increased vascular function and arterial remodeling and a general decrease in arterial stiffness. In short, stretching improved blood flow mechanisms leading to better cardiovascular health in study participants.
So, instead of focusing on peak performance, pushing yourself to the limit, or “feeling the burn,” here are four other exercises that have been scientifically proven to produce serious benefits without a serious commitment.
Yoga
The aforementioned study was far from the first to point out the cardiovascular benefits that come with regular stretching. Regular yoga sessions, for instance, may be a boon to health in a number of other ways.
Regular yoga practice can help reduce inflammatory markers. This is important because high levels of inflammation are associated with all-cause mortality. The authors of one study of more than 200 participants found that inflammatory markers (TNF-α and IL-6) linked to coronary heart disease, depression, type 2 diabetes, arthritis, osteoporosis, and Alzheimer disease were all lower in those who were regular yoga participants.
Additionally, cholesterol levels were significantly lower in those who practiced yoga. Other studies have also noted marked lower levels of cholesterol in those who practice regular yoga, including one study that found just 1 year of yoga reduced cholesterol levels by almost a quarter.
Various studies have found that yoga lowers blood pressure, helps the regression of coronary lesions, and offers a range of other physical benefits, as well as promoting mental well-being.
In fact, one review of more than 80 studies concluded that, in most cases, yoga interventions appear to be equal or even superior to physical exercise in improving a variety of health-related outcomes, including heart rate variability, blood glucose, blood lipids, salivary cortisol, and oxidative stress. Yoga practitioners also report improved measures of fatigue, pain, and sleep. With a number of free resources, like YouTube channels, to help get you started, yoga may be the perfect way for the workout-averse to look after their health.
Walking
Of course, the idea of twisting like a pretzel on a yoga mat won’t appeal to everyone. Perhaps you’re feeling cooped up and need a change of scene, but you don’t feel like tackling a 10K run just yet. Well, walking may be your answer.
For decades, studies have linked even low- to moderate-intensity physical activities, like walking, to important cardiovascular health benefits and the prevention of heart disease. Studies have shown that simple brisk walking can help reduce anxiety and tension, promote weight loss, improve cholesterol levels, and slow the progression of osteoporosis.
This line of inquiry remains ongoing. Last year a study looked at the effect of walking on the risks of all-cause mortality in older women. After analyzing the walking habits of over 16,000 people, researchers found that as few as 4,400 steps per day was significantly related to lower mortality rates. Mortality rates further decreased with up to 7,500 steps per day.
With study after study finding associations between regular walks and boosts to cardiovascular health, there’s no time better than now to start finding the best local trails or parks in your area. Some studies suggest aiming for 150 minutes of walking per week or having a target of 10,000 steps per day.
Strength training
Don’t panic—strength training doesn’t have to mean bodybuilding or aiming for a six-pack. If you’re a beginner, strength or resistance training can start slow, with as little as 20 minutes per session when you start out. The key is not to push yourself to the max, but to find a comfortable level of working out and being consistent with your routine. This means completing reps with some effort but not to the point where you’re grunting or straining.
Strength training can be done in your own home and doesn’t require you to run about and get out of breath (though your muscles will ache a little). It also offers a number of health benefits, some of which may surprise you.
You know, of course, that resistance training can help build muscle, burn fat, and increase metabolism. Likewise, strength training can improve cardiovascular health by lowering cholesterol and promote healthy bones by reducing certain aging factors in skeletal muscle. Also, having stronger, denser bones is particularly important for aging populations and can reduce the risk of developing osteoporosis.
But, did you know that a number of studies have also demonstrated that this kind of training can improve glycemic control and insulin sensitivity, and help in the prevention and management of type 2 diabetes?
Other studies have established a link between strength training and improved cognitive abilities. A study published in Molecular Psychiatry examined whether a 6-month strength training regimen would have any impact on 100 older individuals who were at risk of developing dementia. The authors found that the training led to a thickening of grey matter in the posterior cingulate cortex, a key part of the brain that is affected in the early stages of Alzheimer disease. They concluded that resistance training could be a key part in helping to combat the effects of aging as well as Alzheimer disease.
But, again, the key is to find a routine and stick to it. If you do, you should experience noticeable gains within 4 to 8 weeks.
Tai chi
If strength training seems a bit too gung-ho, there are far more peaceful ways to address your fitness levels. For those who prefer to take things a little slower and more gently, tai chi could be the perfect activity.
While it won’t leave you out of breath, tai chi can improve muscle strength, flexibility, balance, and even aerobic conditioning. Due to the unsupported arm exercises involved, tai chi can be as good for upper body strength as resistance training when practiced regularly.
One review article of randomized clinical trials concluded that “consistent, significant” evidence exists that tai chi can provide a number of health benefits. The authors found that these benefits relate to a number of physiological areas, including bone health, cardiopulmonary fitness, immunity, and balance.
Another study looked at 30 college students and the impact that 3 months of regular tai chi had on their overall physical and mental health. The addition of tai chi was found to significantly improve a variety of aspects of participants’ health, including general health, levels of bodily pain, vitality, and mental/emotional health.
Summer 2020
“It’s Hot-Hot-Hot”
If it were cold in July, no one in the North East would be happy. Then again many of us are equally not thrilled when the weather people start to report a “Heat Wave” is about to settle in to the Delaware Valley. But this summer has started and it is “Hot-Hot-Hot”. So everyone must be aware of the dangers of the summer heat. So here are some useful tips to live by.
Stay Cool
- Stay in air-conditioned buildings
- A fan alone is not enough to cool your home during extreme temperatures
- Limit outdoor activity, especially during the hottest part of the day
- Avoid direct sunlight
- Wear loose, lightweight light-colored clothing
- Take cool but not cold showers to lower your body temperature
- Check on at-risk friends, family and neighbors at least twice a day
- Never leave infants, children, pets or the elderly in a car or truck – even a few minutes is too long
Stay Hydrated
- Drink more fluids than usual even if you are not exercising
- Don’t wait until you are thirsty before you drink
- If your doctor usually limits the amount you drink or you are on water pills, call to ask how much you need to drink during the extreme heat.
- Drink 2 – 4 cups of water every hour if you are working or exercising outside
- Avoid alcohol or liquids with sugar
- Check to be sure your family, friends and neighbors are drinking enough water
- Make sure pets have water available
| Heat Exhaustion Symptoms | What to Do |
|
· Heavy Sweating · Weakness · Skin cold, pale & clammy · Weak pulse · Fainting, vomiting |
· Move to cooler location · Lie person down, loosen clothing · Use cool, wet cloths on body or a bath to lower temperature · Sip water if you vomit and if it continues, get medical care |
| Heat Stroke Symptoms | What to Do |
|
High body temperature [above 103 F] Hot, red, dry or moist skin Rapid & strong pulse Possible unconsciousness |
THIS IS A MEDICAL EMERGENCY – CALL 911 Move person to cooler area Lower person’s temperature with cool cloths or bath Do NOT give any fluids |
People who work outdoors are more likely to become dehydrated and are more likely to get heat-related illness.
STOP
All activity and get to a cool environment if you feel faint or weak.
- Drink from two to four cups of water every hour while working. Don’t wait until you are thirsty to drink.
- Avoid alcohol or liquids containing large amounts of sugar.
- Wear and reapply sunscreen as indicated on the package.
- Ask if tasks can be scheduled for earlier or later in the day to avoid midday heat.
- Wear a brimmed hat and loose, lightweight, light-colored clothing.
- Spend time in air-conditioned buildings during breaks and after work.
- Encourage co-workers to take breaks to cool off and drink water.
- Seek medical care immediately if you or a co-worker has symptoms of heat-related illness.
- For more information, please visit: http://www.cdc.gov/niosh/topics/heatstress/.
Remember your body is about 60% water and you need to keep it that way especially during the summer heat. Hydrate all day long and stay healthy.
Happy Summer!
Dr. Lee Ann
Spring 2020
State of NJ testing guidelines for COVID 19as of April 28, 2020 – Download Here
COVID 19 can cause increased Stress and Anxiety
How can we get through this pandemic?
Watch our podcast on our website regarding anxiety. https://www.pinestreetfamilypractice.com/podcasts
- Exercise
- Watch diet
- Deep breathing
- Meditate, rest
How can we exercise if we are inside?
- If you have stairs in your house safely walk up and down, time yourself goal of 5 minutes
- Walk the perimeter of your house inside or outside at a safe distance, time yourself goal at least 15-20 min a day
- Get everyone involved, make it fun create a family seek and find within your house
- Do puzzles either word or pieces helps keep the mind occupied
- Play board games, this gets the family involved
How can we watch diet, food may be limited?
- When shopping limit high fat saturated foods and sweets purchases try to plan meals so can included fruits/veggies
- Make sure you are staying hydrated 6-8 glasses of water a day
Deep breathing
- Take 3 deep breaths
- Slowly inhale and control exhale
- Make sure your chest is moving up during inhales
- Slowly count to 30 (if you can) when exhaling on the 3rd breath
Meditate
- This is difficult and you will need to concentrate and practice
- Breathe deeply, be in a quiet area and get into a comfortable position
- You will need to completely relax while staying awake
- Close your eyes gently
- Put your thoughts aside empty your mind and focus on your breathing
- You will need to practice…try 10 minutes a day…you deserve it
Rest
- We need to try and sleep between 6-8 hours a night
- Try not to listen to social media and news constantly
- Reduce stimulus 30 minutes before bed no phone or v
Different Therapies
- Art therapy…try drawing, doodling, or coloring
- Music therapy…listen to your favorite artist
- Dance therapy…dance like no one is watching
- Pet therapy…if you have animals playing and/or petting them can be very relaxing
- Guided image therapy…close your eyes, go to your happy place, either the beach, the mountains, the park or some place that you feel comfort, your imagination is limitless!
Try one or try them all, Be Safe!!!
COVID 19
How many times a day do we here COVID 19, social distancing, and wash your hands?
Did most people know what a pandemic was before this virus, most likely not.
COVID 19 is on everyone’s mind and should be, can you remember the last time you didn’t think about this pandemic?
This can often cause increased stress and anxiety. Being prepared, be safe and be cautious, this can help slow the spread.
What do we know about COVID 19?
- COVID 19 is a virus that is spread through droplets by coughing/sneezing.
- Common symptoms are coughing, shortness of breath and fever.
How can we help slow the spread?
- Take precautions
- Wear face coverings
- fit snugly but comfortably against the side of the face
- be secured with ties or ear loops
- include multiple layers of fabric
- allow for breathing without restriction
- be able to be laundered and machine dried without damage or change to shape
- Wash hands for AT LEAST 20 seconds
- Clean surfaces
- High touch surfaces are tables, doorknobs, light switches, countertops, handles, desks, phones, keyboards, toilets, faucets, sinks.
- Stay inside
- Keep 6 feet away from people (social distancing) if going outside for necessary essentials
- Limit going outside see if stores have special hours for senior if you are in that age group
- Wear face coverings
What to do if you are feeling sick:
- If you think you may be sick, stay home and consult with your healthcare provider, telemedicine options are available at Pine Street Family Practice.
- Rest, increase fluids to stay hydrated, take Tylenol as needed
If you are very sick get medical attention immediately
If you develop any of these emergency warning signs* for COVID-19 get medical attention immediately:
- Trouble breathing
- Persistent pain or pressure in the chest
- New confusion or inability to arouse
Call 911 if you have a medical emergency: Notify the operator that you have, or think you might have, COVID-19. If possible, put on a cloth face covering before medical help arrives
At Pine Street Family Practice, we care about YOU!
The safety and health of our patients, staff and providers are our top priority while continuing to provide you with quality medical care.
Be safe!
Winter 2020
Eat Smarter in 2020
There are very few of us who don’t want to lose a few pounds. Here is an overview from US New & World Report 2020 rankings. Please remember that “Diets Don’t Work!”. Consistency in an eating habit that you can sustain on a weekly basis over months is the hallmark of successful long-term weight loss and healthy eating. This prevents the yo-yo dieting and then the need for you to continue to lose the same 40 pounds over and over. Read, eat and enjoy 2020.
– Dr. Lee Ann

This is the 10th year US News & World Report has published its “Best Diets” ranking. The full report includes 35 plans, both well recognized and not-so-familiar. Primary care patients looking to make lifestyle changes, lose weight, or give their food choices a jolt have been scrolling through the offerings and the extensive information on each since publication on January 2, 2020.

#1. The Mediterranean Diet. The popular diet is low in red meat, sugar, and saturated fat, high in produce, nuts, grains, olive oil and fish. It was also ranked #1 in Best Plant-based Diets and Best Diabetes Diets and #2 in Best Heart-healthy diets.

#2. The DASH Diet, aka Dietary Approaches to Stop Hypertension, is promoted by the National Heart, Lung, and Blood Institute and was designed to prevent hypertension. The focus is on foods high in nutrients that work against high blood pressure, e.g., potassium, calcium, protein, and fiber. The food plan sets a daily sodium limit at 2300 mg/day with a target of 1500 mg for those who stick to it. DASH was also ranked #1 in Best Diets for Healthy Eating and #2 in Best Diabetes Diets.

#3. The Flexitarian Diet. The Flexitarian approach to eating combines vegetarian food choices with a flexible approach to meat consumption. It suggests adding a food group called “new meat” when meal planning to include non-meat proteins such as eggs, beans, and peas. As a weight-loss plan it maxes at approximately 1500 cals/day. It also tied for 2nd place as Best Plant-based and Best Diabetes Diet and was ranked #2 in Easiest Diets to Follow.

#4. Weight Watchers (aka, WW). The original Weight Watchers program focused on weight loss and has always combined in-person meetings with healthful eating. The new myWW program is the easiest to date to customize with its system of Smart Points and the guiding philosophy is a holistic one focused on healthy eating and exercise. The WW plan of eating scored the highest for Best Overall Weight Loss and Best Fast Weight Loss as well as #1 in Best Commercial Diet Plans.

#5. The Mayo Clinic Diet. This diet was developed to help individuals lose weight by recalibrating eating habits and other lifestyle choices. The Mayo Clinic’s unique food pyramid guides selection and emphasizes fruits, vegetables, and whole grains – foods with low energy density. Following the diet, individuals are expected to lose 6 to 10 lbs. in 2 weeks and continue dropping 1 to 2 lbs. until goal weight is reached. The diet tied for the #2 spot in Best Diabetes Diets.

#5 (tie) The MIND Diet, aka, Mediterranean-DASH Intervention for Neurodegenerative Delay. MIND combines the 2 healthy diets and focuses on choices from each that potentially affect brain health, thus reduce the risk for Alzheimer disease. The food plan, rich in leafy green vegetables, nuts, and berries, was found in a 2015 study to reduce Alzheimer risk by 35% for those who adopted it moderately and 53% for individuals who followed it rigorously. MIND was also ranked #3 in Easiest Diets to Follow.

#5 (tie) The Volumetrics Diet. Conceived by a Penn State nutrition professor, Volumetrics is described as less a structured diet than an approach to eating. It focuses follower’s attention on choosing foods with low energy density–foods that tend to fight hunger. While the plan can be followed prescriptively, individuals are encouraged to apply the basic philosophy throughout the day, replacing high-density foods with low-density options. The Volumetrics Diet tied for the #2 spot in Best Weight-loss Diets.

#8. TLC Diet. The Therapeutic Lifestyle Changes diet was created by the NIH’s National Cholesterol Education Program. The focus is on reducing cholesterol intake to promote heart health. The broad eating guidelines recommend fruits, vegetables, cereals, and pasta; low-fat dairy, skin-off poultry. To lower LDL-C, calorie goals are 2500/day for men and d a 1800/day for women; for weight loss daily calories go down to 1600 for men, 1200 for women. TLC was ranked #4 (tie) in Best Diets for Healthy Eating and #5 in Best Heart-healthy Diets.

#9. The New Nordic Diet. The diet is based on 10 concepts meant to “revolutionize” Nordic cuisine and improve public health, among them include more food from the seas and lakes and from wild landscapes. The regimen’s carbohydrate/protein ratio (2:1) relies on a combination of low-glycemic index and moderately high protein foods. It tied for 3rd place in the Best Plant-based Diets.

#9 (tie) The Ornish Diet. Created in 1977 by physician Dean Ornish, founder of the Preventive Medicine Research Institute, the diet is low in fat, refined carbohydrate, and animal protein–a whole foods, plant-based regimen. The food plan was originally conceived to reverse heart disease and proven to do so in randomized controlled trials. The Ornish philosophy emphasizes exercise, stress management, and relationships as part of a heart-healthy way of life. The diet was ranked #1 in Best Heart-healthy Diets and tied for #3 in Best Plant-based Diets.

#9. The Vegetarian Diet. Among people who prefer a vegetarian food plan, the lacto-ovo approach is the most popular. There are US dietary guidelines that provide a template for a healthy plan including how many meatless calories should be consumed and what types of food those should come from. A gradual approach to this way of eating could include a few meatless meals a week. Vegetarian diets have been associated with lower BMI, LDL-C, and glucose levels as well as lower rates of ischemic heart disease.


November 2019
The Best Skin of Your Life!
Did you know skin is the human body’s largest organ? So, taking exceedingly good care of your largest organ is very important. At Pine Family Practice we want to provide our patients with the best non-invasive options for preventative skin care maintenance/cosmetic improvements. Read on and we’ll take a dive into our skin care treatment options.
Up first is our HydraFacial treatment. This is our favorite way to get glowing! If you have not had a HydraFacial yet, you are surely missing out. In fact, HydraFacial was crowned the most popular beauty treatments of 2019 according to Yelp. So, what exactly is a HydraFacial? What sets HydraFacial apart from other facials is the use of spiral design HydroPeel Tips in conjunction with patented vacuum technology and super serums to create a vortex effect to easily dislodge and remove impurities while simultaneously supplying hydrating solutions onto the skins surface. In other words, it takes out the bad and puts in the good. Say goodbye to blackheads, dead skin cells and clogged pores and say hello to beautiful radiant skin.
HydraFacial provides 3 steps in as little as 30 minutes delivering you instant, long lasting results that you can see and feel.
- Step 1: Cleanse + Peel: Uncover a new layer of skin with gentle exfoliating and relaxing resurfacing
- Step 2: Extract + Hydrate: Removes debris from pores with painless suction. Nourish with intense moisturizer that quenches the skin
- Step 3: Fuse + Protect: Saturate the skin’s surface with antioxidants and peptides to maximize your glow
HydraFacial is for all skin types, ages, and tones and addresses all skin care needs including:
- fine lines and wrinkles
- elasticity and firmness
- even tone and vibrancy
- skin texture
- brown spots
- congested and oily skin
- enlarged pores
- dry skin
Treat yourself to a HydraFacial for the best skin of your life!
Gift certificates available for you or your favorite person.
We Recommend a HydraFacial monthly for maximum benefits.
Another amazing skin care treatment option that we offer at Pine Street Family Practice is Exilis Ultra 360. Exilis Ultra 360 targets your skin’s fine lines and wrinkles by safely delivering radio-frequency and ultrasound energy to heat up the skin to stimulate collagen production. What’s even more amazing is Exilis Ultra 360 can be used almost anywhere on the body providing a true head to toe treatment. If you are looking to tighten and tone your body non-invasively with no downtime Exilis Ultra 360 is the easy answer. This treatment like HydraFacial is ideal for anyone! Typically, patients undergo between 4 to 6 treatments scheduled 7-14 days apart. Each treatment of a specific body part usually takes between 15 – 30 minutes. I would describe the treatment as being comparable to a pain-free, hot stone massage. You can easily relax during the procedure as one of our certified technicians will provide you with soothing spa music, aromatherapy and dimmed lighting to maximize your comfort and enjoyment!
Having trouble deciding which one may be better for you? No worries! HydraFacial and Exilis Ultra 360 complement each other producing a more youthful, radiant you. We even provide you with discounted package rates when you purchase the two treatments together because we believe you shouldn’t have to choose. Gift certificates also available!
Mention to our technician that you read our Hot Topic-The Best Skin of Your Life! And receive a free Signature HydraFacial or Exilis maintenance treatment with purchase of a HydraFacial or Exilis treatment.
If you have any questions/concerns or would like to schedule your appointment please give the office a call.
856-629-7436.
YOUR SKIN WILL THANK YOU!
YOU DESERVE IT!
September 2019
Update on Vaping
If you read our prior article on Vaping you understand it is NOT an alternative to quit smoking in fact the most recent information about Vaping is that it is causing unexplained lung illnesses.
In a recent update from the CDC this month September 2019, there have been 6 deaths linked to vaping within ages 18 to 25 and over 450 people experiencing unexplained lung infections. With more than 25 states reporting possible cases of lung illnesses associated with use of e-cigarette products.
While many of the patients, not all, stated recent use of THC-containing products, some described using both THC and nicotine containing products. A smaller group reported using nicotine only.
There has been no evidence of infectious diseases identified in these patients, as a result lung illnesses have been associated with a chemical exposure from vaping. The common factor in these unexplained illnesses has been vaping.
The CDC and FDA are partnering to get to the bottom of these strange illnesses with the recommendation of stopping this habit now.
If you do vape think twice, you are encouraged to monitor for sudden symptoms of cough, shortness of breath, chest pain, nausea, vomiting, abdominal pain, and fever and promptly seek medical attention. E-cigarette products should not be purchased off the street and not be modified by adding THC containing products. E-cigarette products should never be used by youth, young adults, pregnant women, or adults.
Again, if you are interested in quitting smoking, pick a date, develop a plan and ask a provider at your next visit to Pine Street Family Practice.
Here is a hotline number: call 1-800-QUIT-NOW (1-800-784-8669)
Additionally, if you are concerned about your health after vaping or using an e-cigarette product, contact your health care provider, or you can also call your local poison control center at 1-800-222-1222.
Summer 2019
Vaping
Have you ever heard of Vaping or Juuling? Is Vaping the same as smoking? Is there nicotine in vaping? Is it better to switch from smoking cigarettes to vaping?
All good questions.
You most likely have heard of this if you are a teen or young adult.
E-cigarettes are an electronic device that is used to heat a liquid to produce a mist or vapor of small particles in the air. This liquid has nicotine, chemicals, and other flavorings like cucumber, mango, and fruit medleys, making the product more attractive, especially to adolescents. They come in many different shapes and sizes, having a battery or heating element. The devices can have different shapes and sizes, looking like a pen, a cigarette, a cigar, a pipe or every a USB flash drive. They also have different names like e-cigs, vape pens, e-hookahs, or tank systems, it’s also known by its most popular names of vaping or JUULing. JUUL being a common e-cigarette manufacturer and has been around the longest since 2015. Below are a few pictures of what the devices can look like.

A JUUL device is shaped like a USB drive and has the highest percentage of nicotine, according to the manufacturer 1 JUUL cartridge can contain as much nicotine as 20 cigarettes. Adolescents have been reportedly vaping in bathrooms and classrooms. Adolescents and young adults do not understand that vaping is still delivering nicotine causing the addiction. This chemical can alter a young brain which is still developing to age 25. This can cause problems with attention, learning, mood and impulse control. Marijuana can also be used in these devices. Adults and children have been poisoned by ingesting the liquid aerosol and getting the substances in the eyes or on the skin which can be very harmful. There have been many cases where the batteries in the e-cig have been reported to have caught on fire or explode.
Using e-cigarettes is not a good alternative to smoking, there are similar health risks with this product as with smoking tobacco cigarettes.
E-cigarettes and Vaping are not safer then tobacco cigarettes and should not be started.
E-cigarettes cannot help you stop smoking tobacco cigarettes you just switch addiction.
If you are interested in quitting smoking, pick a date, choose a plan and ask a provider at your next visit at Pine Street Family practice.
Here is a hotline number: call 1-800-QUIT-NOW (1-800-784-8669)
Set a good example be tobacco and smoke free!
New Year Resolutions Gone Bust
So, January is gone, the snow is has come and many of our New year resolutions for health have faded. We come out of the gate like gang busters but soon find that we cannot maintain such a frantic pace. One missed gym day turns to two. One piece of pizza becomes three. We are quickly falling back into our old habits. Sometimes we just take on too much at once, feel overwhelmed and quit.
Here is a list of 10 things that we can easily try to lead a healthier life. The good thing is none are overwhelming to try. Would recommend picking a few to try, not all ten at once. Slowly try working your way through the list.
1. Drink Water: When eating a meal water will take up the same amount of space as any liquid, without the empty calories.
2. Don’t Only Drink a meal: Liquid shakes sound healthy but very quickly leave the stomach. This makes our full sensation go away faster.
3. Plan Meals: It is easier to eat healthy if you plan ahead. Waiting to the last minute makes it easy to impulse eat whatever is fastest.
4. Fresh Foods: Avoid eating prepared foods as much as possible. There are usually all kinds of added sodium, preservatives and fat hidden in them.
5. Fruits/Veggies: Have a fruit or vegetable with every meal. Not only are they healthy choices but high in fiber. Fiber gives us a longer sensation of fullness.
6. Food Log: Write down everything that you eat. It’s amazing that when you write it down it makes you think about before you open your mouth again.
7. Small Plates: We are very visual eaters, we tend to fill the plate that we are using to satisfy our brain. Use a smaller plate and it will trick the brain into thinking we are eating more.
8. Cardio 30: Try to get 30 minutes of cardiovascular activity in 3 times a week. Once you are able to do that then try to slowly increase to daily activity.
9. Sleep: Practice good sleep hygiene and get enough sleep. When we are tired our body gets stressed and makes it more difficult to lose weight. Also when we are tired we often will eat whatever to make us feel better.
10. Go Slow: No one says that you need to do everything at one or do it completely the first day. Slowly build up to the desired goal. Focus on one or two things at a time then move on to your next goal when accomplished.
Here’s to a healthy new year not just January!! Dr. Steve
“The Rich Man’s Disease”
How does your blood level measure up to your blood bank account?
Gout is a medical problem that was known hundreds of years ago and also to this day as the “Rich Man’s Disease or the Disease of Kings”. This is because gout has the reputation of being caused by the overindulgence of rich, fatty, and creamy foods, as well as, red meats and expensive shell fish while washing them all down with extreme volumes of beer and wine. So why do some people get gout and some not? The theories continue to abound, but genetics appear to have a key role.
The symptoms start usually with a sudden onset of an extremely painful joint that is red, hot and swollen. Most commonly the big toe, but any joint can be affected. It would not be unusual for this problem to awaken one from sleep and have difficulty walking due to the pain. The joint becomes so sensitive, having the bed sheet or the shoe touching the foot is intolerable.
Gout is the result of the body not being able to process the dietary breakdown of purines turning to uric acid, as well as, the metabolism of alcohol and sugary beverages that increase the production of uric acid. This elevation of uric acid in the blood then circulates and settles in the joints causing this painful joint syndrome.
High uric acid levels in the blood are usually > 6mg/dl in women and > 7mg/dl in men.
What are the dietary triggers of Gout?
Alcohol– in large consumption, alcohol is a known trigger, however even moderate amounts may increase the risk in people prone to gout. Beer is the highest risk and wine appears to be the lowest.
Sugar– sweetened Beverages- high consumption of dietary sweeteners used in common beverages has been known to increase blood uric acid level. Juices with high fructose corn syrup and soft drinks are also known triggers. Natural honey sweetened beverages included in many teas also may increase the uric acid level.
Purine Rich Meats– High intake of purine rich meats may increase a gout attack by 5 times the normal. Red meats- beef, veal, lamb are the highest. Wild game – turkey and duck should also be limited in the diet. Organ meats, like liver, heart and kidney also have elevated levels of purine and can trigger a gout attack.
Fish and Shellfish– Haddock, anchovies, tuna, herring , codfish and trout are all high purine non shell fish that should be avoided with increased risk or prior diagnosis of gout. Mussels and scallops are the highest shell fish to trigger gout, but shrimp, crab and lobster should also be limited.
Tomatoes– This fruit, although a food always mislabeled as a vegetable, has now been labeled a “possible trigger” for gout due to the phenolic acid and glutamate in the tomatoes which then may increase uric acid levels. So over indulgence in tomatoes may also be an avoidable trigger for that chronic gout suffers.
What is the treatment of gout?
I don’t have to be a doctor to give this antidote!
Avoid the TRIGGERS! Alcohol, sugary beverages, red meats, shell fish and some non shell fish, and tomatoes.
For those patients who are unable to comply with dietary treatment the use of colchicine, NSAIDS, prednisone, and allopurinol are the most common treatment options. Cherry juice, drinking more water to keep the body hydrated, rest of the joint, and weight loss are all touted to help prevent uric acid build up in the blood stream and prevent gout attacks.
So as we approach this holiday season and may be treating ourselves to the Trigger List Foods and Beverages- Beware of the King’s Disease and watch your dietary bank account! This is not a “No pain no gain” eating plan. You will pay for your indulgent choices. Choose wisely!
Happy Holidays!
Dr. Lee Ann
We all love when the calendar turns to summer so we can get outside and have fun. Who doesn’t enjoy the sun and the beach. We just need to be prepared for our summer time fun.
First off when the temperature hits the 80-90’s and the humidity rises we need to prepare before going out. Everyone thinks about being well hydrated when exercising or doing yard work. Pre-hydrating when going to do something physically active is important, not only water but sports drinks as well. By the time you start to feel thirsty you are already behind. Symptoms of fatigue, cramping and dizziness are early signs. Headaches, confusion and nausea/vomiting are late signs. Stopping the activity, cooling off and rehydrating are the mainstay of treatment. Symptoms of fatigue and malaise can last for a couple days post heat exhaustion. Heat stroke includes rapid pulse, excessive sweating and passing out. Heat stroke requires intervention with IV fluids to help turn the tide in a hospital setting.
It is graduation and picnic season we need to be vigil for the very young and old. Children and seniors do not tolerate the heat as well because their reserves are less. So it is not out of the ordinary for these groups to suffer heat symptoms at a backyard party. Seniors should be in the shade and drinks readily available for them. Young children have to monitored when playing a lot because of course they do not want to stop to eat or drink something, unless it is ice cream. Keeping an eye on these groups can prevent problems.
Our second big problem in the summer is the sun exposure to our skin. We all want that radiant golden tan but not all of us can attain this. We can get a sever sun burn though. It is important to apply sun screen prior to going out in the sun. We should also re-apply every time that we go into the water. Sunscreen is resistant, there is no such thing as water proof. Reapplication is also recommended after a few hours as it starts to wear off, sweat off or rub off.
Sunburns are not only a problem now but put us at risk for skin damage leading to skin cancer down the road. We pay in our 50-60’s for our beautiful tans in our 20-30’s.
Have a wonderful Summer!! Stay safe stay hydrated and use sunscreen!
Dr Steve

Melt Away the Winter Fat Get Ready for Summer

Now Available at Pine Street Family Practice
As we move from our warm and cozy homes and bulky clothing of this cold winter it is time to think about warming up and moving into the spring season. What comes next? It is the fun and sun of summer and removing those layers. Many of us can’t wait for the pool and shore months, but this means we need to start to get ready for bathing suit season. Some of you have made New Year’s resolutions and have started your new eating and exercise routines to shed those extra pounds in anticipation of shedding the layers of clothing. Many of us have continued our year round health mantra and would still like to see those few extra inches melt away to complement our hard work and dedication at the gym and eating right. So whether you are on a new mission or continuing on your trek to looking and feeling better Pine Street Family Practice has a way to compliment your goals.
is a safe and in office non-invasive procedure that will help you melt away those annoying inches that just don’t want to budge with the diet and exercise program you have implemented. Coolsculpting works by delivering a controlled cooling to gently and effectively target fat cells to crystallize and then die off and be reabsorbed by your body, while leaving the surface skin unaffected. As the targeted fat cells die and become reabsorbed that specific area of fat then flattens and those inches become reduced to help you achieve the sculpted inch reduction you desire. This process will take 8-12 weeks to see the full improvement you want and will be reassessed in our office at that time. Areas of the body with best results are the abdomen, triceps, front of chest arm fat near the arm pits, back fat, under the chin, outer and inner thighs and the buttocks (banana roll) areas. I know we all have one of these areas that could use some inch reduction!
Pine Street Family Practice has fully trained staff that will do a free in office consultation to evaluate which body areas you are interested in sculpting and help you identify other areas that will be improved with this procedure. Not all fat is “freezeable” fat and not all areas you may want inch reduction will have good results, so a consultation is necessary for you to understand the process and achieve the desired outcome. We have financing options also available to help you make this process more attainable for you.
Go to our Facebook page and see my pictures of the procedure from February 2018 and the progress I have made. Call our office to schedule a free consultation now and continue the process to a healthier and more sculpted you.
Dr. Lee Ann
SHINGLES
Do you know someone who has had Shingles? Chances are you have heard of it but do you really know much about the virus. We are Pine Street Family Practice think it’s important for you to know a little bit about the virus and how you can help protect yourself.
WHAT IS SHINGLES?
Shingles is a viral infection that can cause a very painful rash. This blistery rash can appear almost anywhere on the body which shows up on one side. The virus’ name is varicella-zoster which is the same virus that causes chicken-pox. After you have chicken pox this virus can lie dormant in the nervous system, until it rears its ugly painful head, at what age – not known, where on the body – can be anywhere, how long does it last – undetermined.
WHAT ARE THE SIGNS AND SYMPTOMS?
Some signs and symptoms include fluid filled blisters either in a linear pattern or a group that can be red, itchy, tingly, and painful. This rash can be very sensitive to the touch. Although this virus is not life threatening if the rash develops near the eyes this can be very serious and the pain can be debilitating. Some people have complained of fever, fatigue, headaches, and becoming sensitive to light. This virus can be contagious if you come in contact with an open blister.
WHO CAN GET SHINGLES AND HOW BAD CAN IT BE?
The shingles virus does not discriminate, male or female, young or old, healthy individuals or people who have compromised immune systems. Complications associated with this virus are vision problems, post herpetic nerve pain, and possible neurological problems, like inflammation of the brain or hearing problems.
SO WHAT’S THE BUZZ ABOUT SHINGRIX?
There are 2 vaccines that were developed, Zostavax and Shingrix.
*Zostavax was approved for use in 2006, it’s a one dose vaccine recommended for people over the age of 60 with an 65% effective rate.
*Shingrix was approved for use in 2017 and is the preferred alternative. This is a two dose vaccine for people ages 50 and older, with the second dose given anywhere from two to six months after the first dose has been administered. And if you’ve received the Zostavax vaccine already you can also receive the Shingrix vaccine. The most common side effects of the vaccine is a headache, redness, itching and soreness at the injection site.
A FEW QUESTIONS:
-Who can get the Shingrix vaccine? Anyone over the age of 50, it’s a 2 dose series.
-Can I get the Shingrix vaccine if I receive the Zostavax already? Yes you can.
-How can I get the vaccine? Call the office we ask that you call your insurance company and give them code 9750 and see if the vaccine is covered. Then call our office and schedule a convenient time.
-Why should I get the Shingrix vaccine? In people ages 50-69 the vaccine was 95% effective in preventing shingles and over 90% effective in preventing the pain associated with the rash. In ages 70 and over the vaccine was almost 90% effective.
As we get older our risk of getting shingles increases.
So why get ShingRix-it will help prevent the after-shingles pain that can last for six weeks to six months and in some people, it can last a lifetime.
Protect yourself today! Call the office for an appointment.
OVER 70? Four Test to Avoid
If you’re over 70, regular screening tests — especially when it comes to cancer — may be a big waste of time, say a growing number of health experts worried about the over testing of those who are in their 70s, 80s and even older. These experts’ concern is that unnecessary screenings could lead to invasive procedures or treatments that leave patients worse off than before, especially among those with serious health problems such as heart disease.
Colonoscopy
Having a colonoscopy past age 75 may do little to protect you against cancer, reports a new Harvard study of more than 1.3 million Medicare patients ages 70 to 79. Researchers found the cancer risk dropped from about 3 percent to a little more than 2 percent over a span of eight years. At the same time, other studies have shown, the risk of complications from the test increases with age, especially for those in their 80s. The U.S. Preventive Services Task Force (USPSTF), an independent advisory board of medical experts, recommends that screening for colorectal cancer in adults 76 to 85 “be an individual decision,” based on overall health and careful consideration of potential benefits and risks. Obviously, if you’ve had a polyp removed or have a family history of colon cancer, your risk is higher and you should probably be screened. If not, you may be able to finally skip all that lovely laxative prep.
Mammogram
The experts pretty much agree that women should get a mammogram every one to two years until age 75. After 75, however, the evidence for continuing the exams is murky. The USPSTF says there is “insufficient evidence” to conclude yay or nay to mammograms past 74. A large European study of women 70 to 75 showed that screening mammograms may have limited benefits and could lead to overtreatment, putting some women at risk from harmful side effects. For women with several chronic conditions that could affect their life expectancy, the benefits of routine mammograms after 75 are questionable. Those women should discuss with their doctors whether continuing the exams is really necessary.
PSA Test
No medical group recommends a PSA screening for prostate cancer past age 75, yet recent research published in the Journal of the American Medical Association found that 41 percent of men in this age group still have the test, many at the recommendation of their physician. Talk with your doctor, but many men age 76-plus can skip this.
Pap Smear
After age 65, most women with no previous cancer or precancerous lesions are good to go if they’ve had three negative Pap smears to check for cervical cancer in the previous 10 years. Unfortunately, most women have become so accustomed to having an annual Pap smear that they have them even after undergoing a hysterectomy, according to a study. So, ladies, assuming your physician agrees, you can cross this test off your annual to-do list.
Two Test You Should Get
Bone Density Scan
While women should be getting routine bone density scans beginning at 65 (or earlier, depending on their risk factors), men 70 and older also need to get a bone mineral density test to check for osteoporosis. This weakening of the bones is often considered a “silent disease,” because its symptoms can develop unnoticed until a bone fracture occurs. In men, osteoporosis begins later than in women, and progresses more slowly, but the problem is growing among men who are 70-plus, notes the National Institute of Arthritis and Musculoskeletal and Skin Diseases. Indeed, by age 65 or 70, men and women are losing bone mass at about the same rate, making this screening test critical for everyone — men as well as women — over age 70.
Abdominal Aortic Aneurysm Screening
Men 65 to 75 who have been smokers anytime during their lifetimes should have a onetime ultrasound to screen for an abdominal aortic aneurysm (AAA). The aorta, the main artery supplying blood to the body, extends from the chest to the abdomen. Men who have smoked are at higher risk for the aorta to rupture, which is usually fatal, but if an aneurysm is caught before rupturing, it can be successfully repaired by surgery. The evidence is unclear whether routine screening would benefit women ages 65 to 75 who have been smokers in the past, notes the USPSTF, but the panel recommends against AAA screening for women who have never smoked.
Six Things That Raise Your Blood Pressure
American Heart Association News, 02/26/2016
· Salt. The American Heart Association recommends people aim to eat no more than 1,500 mg of sodium per day. That level is associated with lower blood pressure, which reduces the risk of heart disease and stroke. Because the average American’s sodium intake is so excessive, even cutting back to 2,400 mg per day can improve blood pressure and heart health.
· Decongestants. People with high blood pressure should be aware that the use of decongestants may raise blood pressure. Many over–the–counter (OTC) cold and flu preparations contain decongestants. Always read the labels on all OTC medications. Look for warnings for those with high blood pressure and who take blood pressure medications.
· Alcohol. Drinking too much alcohol can raise your blood pressure. Your doctor may advise you to reduce the amount of alcohol you drink. If cutting back on alcohol is hard for you to do on your own, ask your healthcare provider about getting help. The AHA recommends that if you drink, limit it to no more than two drinks per day for men and no more than one drink per day for women.
· Hot Tubs & Saunas. People with high blood pressure should not move back and forth between cold water and hot tubs or saunas. This could cause an increase in blood pressure.
· Weight gain. Maintaining a healthy weight has many health benefits. People who are slowly gaining weight can either gradually increase their level of physical activity (toward the equivalent of 300 minutes a week of moderate–intensity aerobic activity), reduce caloric intake, or both, until their weight is stable. If you are overweight, losing as little as five to 10 pounds may help lower your blood pressure.
· Sitting. New research shows that just a few minutes of light activity for people who sit most of the day can lower blood pressure in those with type 2 diabetes. Taking three–minute walk breaks during an eight–hour day was linked to a 10–point drop in systolic blood pressure.
Is it the Flu or a Cold?
When you wake up sneezing, coughing, achy and feverish how do you know if it is a cold or the flu? It’s important to know the difference between the two because treatments are different. Also secondary health issues can be more serious with one versus the other. For the most part a cold is a milder respiratory illness then the flu. Length of symptoms also varies greatly from a cold to the flu.
Cold symptoms can begin with a sore throat that lasts a couple days. This is often followed by nasal symptoms that can be either runny or congestion. Nonproductive cough is not uncommon. Fever is rare in adults but can be low grade. Children are more likely to have a fever.
Flu symptoms are usually much more severe and come on very quickly. Symptoms can include sore throat, headache, cough and runny nose. Fever is usually high causing body and joint aches.
SYMPTOMS COLD FLU
Fever Seldom, mild Usual, 101-102
Headaches Occasional Common
Body aches Slight Usual, often severe
Fatigue Sometimes Usual, up to 2weeks
Congestion Usual Sometimes
Sore throat Common Sometimes
Cough Mild Moderate/ severe
Complications Sinus HA, Ear Infection Bronchitis/Pneumonia
The best treatment for either is prevention. Good hand washing techniques is the most important prevention, along with avoiding touching your face and staying away from those who are visibly sick. For the flu getting an annual vaccine is important. Cold treatments include decongestants, pain/ fever relievers and cough meds. Flu treatments pain/ fever relievers, decongestants, cough meds and antiviral meds.
Cold symptoms can last for up to a week no matter what you do. The first 2-3 days are the worst and when you are the most contagious. Flu symptoms are much more severe and can last 10-14 days. A not uncommon complication of the flu is pneumonia, which can last for 3-4 weeks after the flu. This is much more common in the young, elderly or people with lung problems.
If you have a cold or the flu and symptoms worsen after a few days, it’s time to call the doctor. Other worrisome symptoms include persistent fever for more than 4 days, chest pain, persistent cough, ongoing sore throat or shortness of breath. Seek the advise of a physician if any of the above symptoms occur.
Mosquito Fever Is Among Us
It is spring, it’s wet and the mosquitoes are on their way. As the weather gets warmer and we plan more outdoor activities, it’s important to remember that we are not the only ones becoming more active. Mosquitoes are vectors for disease. This means they can transmit disease from one human or animal to another. Typically, the diseases are caused by viruses or tiny parasites. The virus and mosquito coexist together without harming each other. The virus reproduces itself within the mosquito, and then is passed along when the mosquito bites another person.
The big story in the news lately has been the Zika virus. The most common symptoms of the Zika virus are fever, aches, rash and red eyes. Most of the time the illness is not severe enough for people to seek medical treatment. For this reason, people may not even realize they are infected. The worry with the Zika virus is mainly for pregnant women. The Zika virus can cause a serious birth defect called microcephaly or other fetal brain defects. The most recent increase in outbreaks has been in South America, specifically Brazil. Also reports from Central America and Puerto Rico have occurred. No local mosquitoes have been found to have the Zika virus in the United States. Cases that have been diagnosed in the U.S. were all related to travel exposure. The Zika virus can be detected by a blood test, but the availability is limited. Tests need to be approved by the state CDC. Treatment is all symptomatic; it is aimed at preventing dehydration, controlling fever and aches.
Prevention of transmission is also important. Transmission has been found to occur through sexual contact. Males who have traveled to areas endemic with Zika virus and have a pregnant partner are recommended to use condoms with any sexual activity throughout the entire pregnancy. Men who have traveled to endemic areas should avoid attempting to impregnate their partner for 3 months post exposure. Women who become pregnant after recent travel to endemic areas should consult their physician for testing. So as you can see it’s a good news story but not something most of us in the state of New Jersey will have much exposure to.
What we do need to be more concerned about is West Nile virus, which does occur in the northeast. Again symptoms are flu like in nature, fever, aches, chills, and diarrhea. In less than 1% of the cases people develop encephalitis or meningitis. These patients suffer from severe headache, neck pain, fever and seizures. Treatment usually entails supportive treatment in a hospital setting.
The true goal with any mosquito borne illness is prevention. Avoiding mosquito bites by using repellants that contain DEET is the mainstay. When weather permits, wearing long sleeves and pants when outdoors at night is beneficial. Mosquito proof your home by fixing screens and keeping doors closed. Reduce the # of mosquitoes in your yard by removing standing water. Also notify the state of any issues with dead birds in your area, which can be a sign of West Nile virus. Some local municipalities may participate in applying insecticides.
All in all mosquito borne illnesses are not that common in our area. A little prevention will go a long way. If you are planning on traveling to areas endemic with mosquitoes check the CDC website to see what specific precautions should be taken.
THE THYROID GLAND
The thyroid gland is a butterfly-shaped endocrine gland that is normally located in the lower front of the neck.
The thyroid gland can be described as a butterfly-shaped endocrine gland that is normally located in the lower front of the neck. The thyroid’s job is to make thyroid hormones, which are secreted into the blood and then carried to every tissue in the body. Thyroid hormone helps the body use energy, stay warm and keep the brain, heart, muscles, and other organs working properly.
Prevalence and Impact of Thyroid Disease
Here are a few statistics about thyroid disease from the American Thyroid Association.
- More than 12% of the U.S. population will develop a thyroid condition during their lifetime.
- An estimated 20 million Americans have some form of thyroid disease.
- Up to 60% of those with thyroid disease are unaware of their condition.
- Women are 5 to 8 times more likely than men to have thyroid problems.
- One woman in 8 will develop a thyroid disorder during her lifetime.
- Most thyroid cancers respond to treatment, although a small percentage can be very aggressive.
- The causes of thyroid problems are largely unknown.
- Undiagnosed thyroid disease may put patients at risk for certain serious conditions, such as cardiovascular diseases, osteoporosis, and infertility.
- Pregnant women with undiagnosed or inadequately treated hypothyroidism have an increased risk of miscarriage, preterm delivery, and severe developmental problems in their children.
- Most thyroid diseases are life-long conditions that can be managed with medical attention.
Facts about the Thyroid Gland and Thyroid Disease
According to the ATA, the thyroid is a hormone-producing gland that regulates the body’s metabolism—the rate at which the body produces energy from nutrients and oxygen—and affects critical body functions, such as energy level and heart rate.
- The thyroid gland is located in the middle of the lower neck.
- Although the thyroid gland is relatively small, it produces a hormone that influences every cell, tissue and organ in the body.
- Hypothyroidism is a condition where the thyroid gland does not produce enough thyroid hormone.
- Symptoms include extreme fatigue, depression, forgetfulness, and some weight gain.
- Hyperthyroidism, another form of thyroid disease, is a condition causing the gland to produce too much thyroid hormone. Symptoms include irritability, nervousness, muscle weakness, unexplained weight loss, sleep disturbances, vision problems and eye irritation.
- Graves’ disease is a type of hyperthyroidism; it is an autoimmune disorder that is genetic and estimated to affect 1% of the population.
Research Advancements in Thyroid Disease
Research funded by the ATA over the past 40 years has accomplished the following:
- Mandatory screening of newborns for congenital hypothyroidism, and early treatment that has prevented mental retardation.
- Cost-effective methods to detect thyroid cancer by screening the 250,000 thyroid nodules developed in Americans each year.
- Groundbreaking work in brain development and thyroid hormone function.
- Promising Graves’ disease genetic research that may lead to improved prognosis and new preventive treatments.
- An experimental drug that may prove useful for treatment and prevention of eye problems associated with Graves’ disease.
For more information, contact the American Thyroid Association.
We thought our patients would find this article helpful:
5 Important (But Rarely Explained) Medical Terms, and What They Mean
By Jeanne Faulkner
No one wants to seem ignorant when they see their doctor, but no one should be expected to be bilingual either. If your doctor’s medical jargon is incomprehensible, you’re not getting your money’s worth. In fact, not knowing what your doctor is talking about can be downright dangerous.
Here are five common terms that patients hear frequently—but often don’t understand.
1. Blood Pressure. When your doctor says your blood pressure is something over something, what is she talking about? She’s referring to the pressure of the blood in the arteries, the result of the heart muscle’s contractions. Let’s say your blood pressure is 120 over 80, which is read as 120/80. The two numbers reflect the first and last heartbeats heard with a stethoscope after a blood pressure cuff (a sphygmometer) is pumped up to restrict blood flow, then slowly released.
- The first number (120) is called systolic pressure and it measures the highest pressure as the heart contracts.
- The second number (80) is called diastolic pressure and it measures the lowest pressure as the heart relaxes.
What should your blood pressure be? If your systolic number is below 120, and your diastolic number is below 80, you have normal blood pressure. Higher numbers can indicate pre-hypertension, or hypertension (high blood pressure).
2. Cholesterol. What if your doctor says you have high cholesterol? Cholesterol is a natural chemical compound produced by the body, a combination of lipid (fat) and steroid. Cholesterol is a building block for cell membranes and hormones like estrogen and testosterone. The liver produces about 80 percent of the body’s cholesterol; the rest comes from diet. When your doctor gives you your cholesterol lab results, you’ll hear three numbers, which are expressed in terms of milligrams (thousandths of a gram) per deciliter (tenths of a liter) of blood (mg/dL).
- LDL (low-density lipoprotein) cholesterol is known as “bad cholesterol,” because high levels are associated with heart disease. LDL levels lower than 100 md/dL are great; levels from about 130 to 160 mg/dL are borderline, and higher levels boost your risk of heart disease.
- HDL (high-density lipoprotein) cholesterol is considered “good cholesterol,” because it prevents the hardening of the arteries (atherosclerosis) by taking cholesterol out of the arteries and depositing it in the liver. An HDL level of 60 mg/dL or more is good. For men, levels below 40 mg/dL and for women, below 50/dL, raise your risk of heart disease.
- Total Cholesterol is the sum total of all cholesterol components in your blood stream. A good total cholesterol level is under 200 mg/dL.
3. Biopsy. If your doctor says you need a biopsy, she wants to remove and examine a tissue sample. Biopsies often help diagnose or rule out cancers, but are also used to identify other conditions. Biopsies may be performed with a needle or a scalpel; they might be minor procedures or require general anesthesia. After a biopsy, your tissue sample will be sent to a laboratory, examined under a microscope, and subjected to any tests your doctor has ordered.
4. CBC and BMP. Your doctor may order these blood tests to help determine your health status. CBC stands for Complete Blood Count, and it measures the amount of several different types of blood cells, including white blood cells (WBCs), red blood cells (RBCs), hemoglobin (HGB), hematocrit (HCT), and platelets in your body.
- WBC: The normal range is between 4,500 and 10,000 cells/mcL, or cells per microliter (millionth of a liter). A higher count usually indicates infection.
- RBC, Hgb and Hct values indicate the presence or absence of anemia (a lack of red blood cells). Normal RBC range for men is 4.7 to 6.1 million cells/mcL; for women, normal range is between 4.2 to 5.4 million cells/mcL. Normal Hgb is between 13.8 to 17.2 gm/dL (grams per deciliter, or tenth of a liter) for men, and between 12.1 and 15.1 gm/dL for women. Normal Hct ranges from 40.7 to 50.3% (in men), and from 36.1 to 44.3% (in women).
- Platelets indicate your blood’s ability to clot. The normal platelet count range is between150,000 – 400,000 platelets per microliter (millionths of a liter).
- BMP stands for Basic Metabolic Panel, a test for sodium, potassium, calcium, and glucose levels, and measurements of kidney function. Your doctor may order this if you’ve had vomiting or diarrhea, or to screen for other types of diseases, including heart and kidney disease.
5. Body Mass Index (BMI). Your BMI is a measure of your weight in comparison to your height. It’s calculated by plugging your height and weight into a formula.
- Normal BMI for adults is between 20 and 25.
- Overweight is 25 to 30.
- Obese is 30 to 35.
- Morbidly obese is 35 to 40 or above.
Don’t hesitate to speak up when your doctor speaks medical-ese. Excellent health care is all about communication and getting the information you need.
